We’ve all heard the debate on the internet and the news in the past few months, should you or should you not vaccinate? As you know, vaccination is giving yourself (or your child) a shot that gives them a killed/not harmful virus in order to stimulate your body’s immune system, making antibodies and thus lessening the chance of getting that disease. However, in recent years parents across the country have gone against vaccinating their kids, stating that vaccination harms you far more than any benefits it may give. You may have your own opinion on this topic, but let’s look at this scientifically.
First, we’re going to be looking at what the null and alternate hypotheses are. The null suggests that the vaccination does nothing, making them useless. More interestingly, there are two alternate hypotheses in this case. Either the vaccination makes you better, or it makes you worse. Regardless, it does affect you in some way, making both an alternate hypothesis. There’s also chance to look out for, perhaps in the form of you getting better/not getting the illness but not due to the vaccination or getting the illness even though you took the vaccination. Reverse causation would mean that getting better or worse makes the vaccination, making it not possible in this case. So, we have three options: The null hypothesis, alternative hypothesis 1 (vaccinations make you less susceptible to illness and disease), and alternate hypothesis 2 (vaccinations make you more susceptible to illness and disease, or make you worse off in some fashion).

Is vaccinating a good thing for you? Source
Background: Obviously, there are multiple ways to look at this question. We can look at how it affects children, how it affects a specific disease, etc. After looking through Google Scholar for some time, I finally found a study I thought would be relevant to us early adulthood students, especially the women of our class. We’re (hopefully) a bit of a way off from having kids of our own and likewise are well past a majority of our vaccinations. However, HPV is something that can significantly affect women at our age, so I believe that should be the focus of this blog. Obviously, the Human Papimillovirus (HPV) is extremely prevalent in young adult women, causing things like an increase in the risk of cancer, especially cervical cancer. This can make young women barren for life, according to this CDC article.
The Procedure: Now, onwards to the study, which happened in Queensland, Australia between 2007-2011. In this study, the researchers vaccinated the women, aged between 12-27 and having their first cervical pap smear, and observed their risk of cervical cancer over the next four years. Obviously, as we discussed in class, this is an observational study. The independent variable is the vaccination given, while the dependent variable is their health in the next four years. It should be mentioned that there wasn’t an ethics problem here, because instead of not giving HPV vaccines to women (which is very unethical and could cause them to get cervical cancer), they limited their participants to those getting a free, first time cervical pap smear, making sure there was no ethical bias. The participants were split into 4 groups based off of age: 11-14, 15-18, 19-22, and 23-27 years. This was used to determine the effectiveness of the vaccinations the older the woman gets. They then judged the data based on of their age, socioeconomic status, and remoteness to take those possible other causes off of the table.
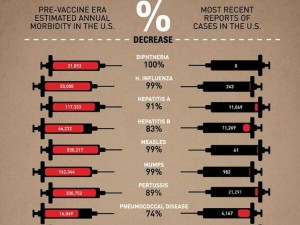
Vaccine has made many diseases decrease between 75-100%! Source
The Results: Comparing the vaccination results to a controlled group of women’s cervical cancer rates. According to the study, there was a 46% reduced rate in high-grade cervical abnormalities amongst women who got vaccinated over those who didn’t, and a 34% reduced rate over any other kind of cervical abnormalities over the control. Needless to say, that is a big difference between the vaccinated and the non-vaccinated. Another major point was that there was a benefit, albeit not a big one, to getting double vaccinated, bumping that rate even higher. The results also showed that the older you got, the less the vaccine helped prevent HPV. That’s quite an interesting finding that the study did not set out to find, but is definitely important in understanding when is the prime time to vaccinate women for HPV to get the best chance of cervical cancer prevention.
So, the data definitely supports the first alternate hypothesis we presented at the beginning of the blog. Indeed, the data clearly shows that the women who took the vaccination were almost half as likely not to get cervical cancer in the next four years. That’s a pretty good increase. In class, we often talk about if this data is guaranteed, or the hypothesis is ruled correct. Well, obviously there are hundreds of studies on the effects of vaccinations, but for this blog we’re only relying on this one source to verify that vaccinations have HPV. However, like Andrew said, the data shown tells you that it would be in your best interest to follow through and vaccinate yourself, especially at the young ages the women in our class.

I appreciate how you took this topic in a unique direction by focusing on the HPV vaccination. I also like how you pointed out that it is possible to still get an illness even after having been vaccinated for it. A few years ago I got the flu even though I had a flu shot that year, and this post made me wonder why that happened. Centers for Disease Control and Prevention offers a couple of explanations. People may actually be infected by a virus with similar flu symptoms, which the vaccination does not protect against. Also, people may have gotten the virus before getting the vaccination, or before it starts being effective. Lastly, the flu vaccination is not consistent in its effectiveness for every individual, so because of this, some people can still get sick.
This article is extremely interesting. My stance on vaccines is simple: if it has worked for many years it is more than likely safe, if it is new do your research. I never got the HPV vaccine because the data on it varies quite a bit. In reference to other vaccines I think everyone should be vaccinated, but I know it’s well disputed and a personal decision. As for me, I will vaccinate my children and continue to get the vaccines I need.